Intestinal Permeability
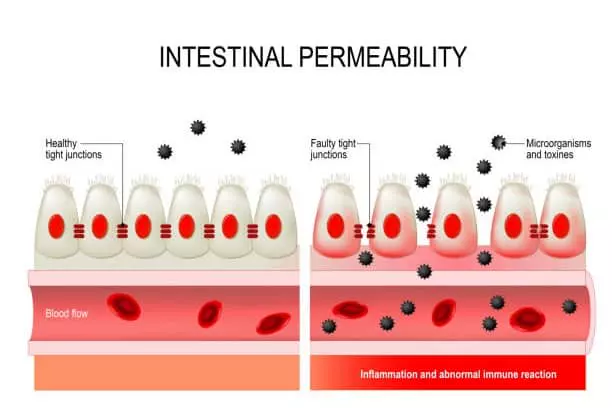
A condition known as intestinal permeability occurs when the junctions in the gut epithelial wall become porous, enabling material from the lumen to translocate into the bloodstream, other organs, or adipose tissue.
Everyone has semi-permeable intestines. Our intestines’ mucous lining is made to allow water and nutrients from food to be absorbed into the bloodstream. However, some persons have hyper- or incleased intestinal permeability. That means their guts let more than water and nutrients through — they “leak”.
Certain chronic gastrointestinal diseases have been linked to leaky gut syndrome, which allows bigger, possibly harmful molecules to pass through. Your intestinal lining’s role in serving as a barrier to bacteria and other infectious organisms inside the gut is one of its primary functions. This barrier is an important agent in your immune system.
See Immune System Booster: 8 Iron-Rich Foods to Eat
Intestinal Permeability and Inflammation
Increased intestinal permeability, sometimes known as “leaky gut,” is linked to a wide range of diseases, including inflammatory bowel disease, dermatitis, autoimmune diseases, food sensitivities, autism, learning disabilities, and many more.
Because the intestines’ damaged barrier allows poisonous substances to enter the bloodstream and poison the body, this “leaky gut” leads to diseases. If a person additionally has intestinal overgrowth of bacteria or a high concentration of certain bacteria that create toxins, this will be exacerbated!
The gastrointestinal tract has two main functions:
- to digest and absorb important nutrients for the body’s growth and function, and
- to act as a barrier to keep harmful substances, immune compounds and microorganisms (bacteria, parasites etc.) from entering the blood.
When the integrity of this intricate system is impaired and there is greater intestinal permeability, illness can quickly arise. Increased intestinal permeability, commonly referred to as “leaky gut,” is linked to a number of diseases and ailments, including autoimmune disorders, autism, food sensitivities, inflammatory bowel disease, and jaundice.
Intestinal Permeability Assessment
Intestinal Permeability Assessment is an effective noninvasive gastrointestinal test assessment of small intestinal absorption and barrier function in the bowel.
The small intestine performs the dual roles of being an organ of nutritional absorption and digestion as well as a strong mechanical and immunological barrier against the overabsorption of bacteria, food antigens, and other macromolecules.
Chronic gastrointestinal imbalances as well as numerous systemic diseases are linked to both malabsorption and increased intestinal permeability (also known as “leaky gut“).
Leaky gut, or increased intestinal permeability, in the small intestine can:
- Increase the number of foreign compounds entering the bloodstream
- Allow bacterial antigens capable of cross-reacting with host tissue to enter the bloodstream, leading to auto-immune processes
- Enhance the uptake of toxic compounds that can overwhelm the hepatic detoxification system and lead to an overly sensitized immune system
There has been evidence of leaky gut in a wide range of diseases, including:
- Inflammatory Bowel Disease (IBD)
- Food allergy
- Inflammatory joint disease
- Chronic dermatologic conditions
According to research, the increased intestinal permeability seen in people with vasculitis, rheumatoid arthritis, and ankylosing spondylitis may play a significant role in the pathogenesis of these diseases.
On the other hand, decreased permeability seems to be the main reason for malabsorption, which leads to malnutrition and failure to thrive. Due to damage to the microvilli, permeability to big molecules may rise in some small intestinal disease states, such as gluten-sensitive enteropathy, whereas permeability to tiny molecules may fall.
As a result, nutrients are even less readily available to help the body detoxify the antigens that are constantly flooding it.
Intestinal Permeability Causes
Increased intestinal permeability, also known as intestinal hyperpermeability, is one potential factor in leaky gut. That may occur if the tight junctions in the gut, which regulate what enters the small intestinal lining, aren’t functioning properly. This could cause substances to enter the bloodstream.
Some of the possible causes of increased intestinal permeability (leaky gut) may include:
- Intestinal infection
- Ingestion of allergenic foods or toxic chemicals
- Deficient secretory IgA
- Trauma and endotoxemia
- NSAIDs
Intestinal Permeability Test
Two non-metabolized sugar molecules’ capacity to pass through the intestinal mucosa is directly measured by the intestinal permeability assessment test. The patient drinks a premeasured amount of lactulose and mannitol.
The amounts of the two sugars recovered in a urine sample that was taken over the course of the following six hours represent the degree of intestinal permeability or malabsorption.
Test Type: UrineTest
Intestinal Permeability Symptoms
One reason intestinal hyperpermeability is not a recognized medical diagnostic today is because there is no established technique to detect intestinal permeability in patients directly.
Intestinal Permeability Treatment
The greatest method to guard against intestinal permeability (leaky gut) may be to practice self-care activities that support general digestive health.
- Increase your intake of high-fiber foods.
- Reduce your intake of refined carbohydrates.
- Reduce your use of NSAIDs.
- Take probiotic supplements.
- Reduce your stress levels.
- Reduce your alcohol intake.
Intestinal Permeability Diet
Eat more prebiotic foods, such as beans, onions, asparagus, oats, bananas, and other foods high in prebiotic fibers. Increase your probiotic intake to help your body produce more good gut bacteria. Yogurt, kimchi, kefir, and tempeh are all examples of foods that have undergone fermentation.
Otherwise, if you have leaky gut syndrome, you should avoid these foods: refined carbohydrates, glutinous grains, white sugar, dairy products, vegetable oils, artificial sweeteners, alcohol, and caffeine.
FAQ
How is intestinal permeability measured?
Intestinal permeability can be measured using the lactulose/mannitol recovery test.
What about malabsorption?
This test not only measures leaky gut but also aids in the diagnosis of malabsorption.It may suggest malabsorption of small molecules and potential intestinal villi atrophy if a low quantity of mannitol, which typically penetrates the intestinal epithelium, is seen. These tests are more accurate if you feel you have fructose malabsorption or lactose intolerance.
How does the test work?
The test works on the principle that small molecules are readily absorbed by the intestinal cells, whilst larger molecules are not. The test involves taking a drink that contains two water-soluble sugars that do not get metabolised by humans.
If absorbed into the bloodstream (via the gut lining) they are excreted into the urine. The mannitol is expected to be absorbed to some extent, but the lactulose should normally be excluded by a healthy gut lining.
When should I consider taking an intestinal permeability test?
Leaky gut (intestinal hyperpermeability) is frequently associated with the following conditions:
- Gut dysbiosis – this can occur for many reasons.
- Irritable Bowel Syndrome
- Small intestinal bacterial overgrowth (SIBO)
- Inflammatory Bowel Disease – Ulcerative colitis, Crohn’s disease
- Coeliac disease
- Fatigue
- Food allergy or intolerance and sensitivities
- Psoriasis
- Excess exposure to anti-inflammatory drugs
- High alcohol intake
Bottom line
Although it might be challenging to distinguish the symptoms of increased intestinal permeability from the inflammation that comes before it, some people actually have this condition. When your gut lining is more permeable, bacteria living in your gut could cross the intestinal barrier, but we don’t know if this does significant harm separate from the original disease or injury that caused it. According to several research, liver disease may be caused by bacteria products that pass from the gut to the liver.
SOURCE: NEWFASTHEALTH CLINIC
Share: