Leaky Gut Syndrome
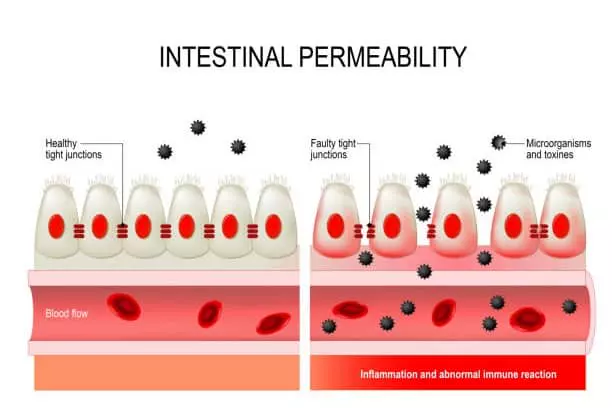
According to the notion known as “leaky gut syndrome,” intestinal permeability has its own independent underlying cause in addition to being a symptom of gastrointestinal disease. The hypothetical ailment known as “leaky gut syndrome” is not yet accepted as a legitimate medical diagnosis. It is predicated on the idea that some gastrointestinal diseases are accompanied with an increase in intestinal permeability.
Toxins may enter your bloodstream if your gut barrier is impaired. These toxins may cause an inflammatory reaction, which may lead to the development of several diseases.
Although there isn’t enough data to support the hypothesis, it does have some appeal as a means of explaining a number of illnesses that we haven’t been able to fully explain. Although intestinal permeability, sometimes known as a “leaky gut,” is a true disorder, neither its existence nor the fact that it contributes to other diseases are known. Currently, there is no recognized medical diagnosis for it.
Also read: How to Improve Gut Health Naturally
What is leaky gut syndrome?
Leaky gut syndrome is a hypothetical condition that’s not currently recognized as a medical diagnosis. It’s based on the concept of relative intestinal permeability.
What is leaky gut? The phrase “leaky gut” is frequently used to describe what occurs when the body’s digestive system becomes dysfunctional. Long-term consequences of leaky gut might include more severe health issues in addition to being unpleasant and bothersome.
Intestinal permeability
Everyone has semi-permeable intestines. Our intestines’ mucous lining is made to allow water and nutrients from food to be absorbed into the bloodstream. However, some persons have hyper- or enhanced intestinal permeability. That means their guts let more than water and nutrients through — they “leak”.
Certain chronic gastrointestinal diseases have been linked to leaky gut syndrome, which allows bigger, possibly harmful molecules to pass through. Your intestinal lining’s role in serving as a barrier to bacteria and other infectious organisms inside the gut is one of its primary functions. This barrier is an important agent in your immune system.
See Immune System Booster: 8 Iron-Rich Foods to Eat
Although it might be challenging to distinguish the symptoms of increased intestinal permeability from the inflammation that comes before it, some people actually have this condition. When your gut lining is more permeable, bacteria living in your gut could cross the intestinal barrier, but we don’t know if this does significant harm separate from the original disease or injury that caused it. According to several research, liver disease may be caused by bacteria products that pass from the gut to the liver.
What disease is associated with leaky gut?
There are diseases that are known to be related to intestinal permeability, and much conjecture surrounds other diseases that could also be related.
Recognized disease associations
Numerous inflammatory and autoimmune diseases of the digestive system, such as celiac disease and inflammatory bowel disease, are known to exhibit intestinal permeability. In these circumstances, scientists typically view it as a symptom rather than a cause.
These diseases cause chronic inflammation in the intestines, which leads to erosion of the intestinal barrier gradually over time.
The intestinal barrier eventually erodes as a result of the persistent inflammation that these diseases generate in the intestines. This has led to some speculation that intestinal permeability might develop independently from these diseases, and might even be a contributing cause.
However, researchers found that intestinal permeability in these instances wasn’t sufficient to develop the disease on its own. It was more likely to be a disease’s first warning symptom.
Possible disease associations
Leaky gut syndrome may have a number of other diseases as a result. The theory is that intestinal “toxins” might escape into your bloodstream and trigger an inflammatory reaction. Asthma, fibromyalgia, arthritis, chronic fatigue syndrome, and metabolic diseases including obesity and diabetes may all be influenced by chronic low-grade inflammation. But the rest remains unclear.
Researchers have shown that individuals with gastrointestinal (GI) diseases, which are known to increase intestinal permeability, had greater amounts of gut bacteria products in their blood. In these situations, inflammation is mostly due to other factors, albeit bacteria-related products may worsen it.
In liver disease, which is directly connected to the gut, they have also measured it. Liver disease may be influenced, but not always caused, by bacteria products that pass from the stomach to the liver through the portal vein.
Who does intestinal permeability affect?
The systematic erosion of the intestinal lining is one of the known causes of intestinal permeability. This is not an easy task. There are several layers of protection in your gut lining.
And while it can be injured temporarily, it is designed to constantly repair and replenish itself. To actually wear it down enough to penetrate the lining requires a significant assault. That typically refers to a long-term disease, drug or alcohol abuse, or radiation therapy.
According to the idea behind leaky gut syndrome, every damage to your gut lining has the potential to cause intestinal permeability if it lasts long enough. Therefore, common everyday factors such as diet and stress may cumulatively wear down your intestinal lining until it becomes permeable.
Although scientists are unsure about this, they do agree that these commonplace elements may cause you to experience uncomfortable GI symptoms and inflammation in the lining of your gut.
How does a leaky gut affect my body?
Intestinal permeability and intestinal lining erosion are two different things. Most patients who suspect they may have a leaky gut have some typical gastrointestinal symptoms such bloating, indigestion, food sensitivities, and abdominal pain.
These types of symptoms are common and may have many possible explanations, and many of them may harm the lining of your intestines. You can have such consequences without having a leaky gut.
Erosion of the intestinal lining
If your gut lining is constantly under attack, it won’t be able to stop bacteria, abrasive particles, or chemical irritants from eroding it. This is what happens in peptic ulcer disease and SIBO (small intestinal bacterial overgrowth). The wrong kind of bacteria overwhelms the other bacteria that would usually balance them.
The erosive acids and enzymes in your gut overwhelm the protective mucus that usually neutralizes them. Erosion of your gut lining will affect your digestion, your immunity, and your sensitivity to pain in your intestines.
And in some cases, it may lead to intestinal permeability. But it doesn’t have to go that far for you to feel unwell. If you have gastrointestinal symptoms, these are likely related to the underlying condition that would be injuring your intestinal lining in the first place. Many gastrointestinal diseases share these same symptoms.
What causes leaky gut?
What is the main cause of a leaky gut? If your intestinal barrier has been damaged, it has likely been under serious attack for a while. The following are the main causes of intestinal permeability:
- Chronic inflammatory states, such as IBD and celiac disease.
- Other diseases that cause intestinal injury, such as HIV/AIDS.
- Chemotherapy and radiation therapies that degrade the intestinal mucosa.
- Chronic overuse of alcohol or NSAIDs, such as aspirin and ibuprofen.
- Food allergies that cause an immune response to certain foods.
Leaky Gut Symptoms
What are the symptoms of leaky gut? No specific signs or symptoms are associated to intestinal permeability. However, intestinal permeability frequently results from damage to your intestinal lining, and you could experience symptoms as a result.
For example:
- A burning feeling of ulceration in your gut.
- Painful indigestion from the loss of intestinal mucosa.
- Diarrhea
- Gas and bloating from fermentation by overgrown bacteria in your gut.
- Low energy from the reduced ability to draw energy from your food.
- Gastrointestinal mucositis from radiation therapy.
Leaky gut syndrome symptoms
- Chronic diarrhea, constipation, or bloating.
- Nutritional deficiencies.
- Fatigue.
- Headaches.
- Confusion.
- Difficulty concentrating.
- Skin problems, such as acne, rashes, or eczema.
- Joint pain.
How is intestinal permeability measured?
Intestinal hyperpermeability is not currently recognized as a medical diagnosis, in part because there is no accepted technique to detect intestinal permeability in patients directly. To seek for symptoms of intestinal permeability in patients, a number of tests are now being investigated in clinical research.
Tests include:
- Urine test. For this test, you drink a solution containing several sugars—some of which are often not absorbed in the intestines—with molecules of various sizes. The amount of sugar in your urine is then measured by experts to determine which sugars managed to get past your gut wall.
- Blood test. This examination looks for signs of gut bacterial invasion in a sample of your blood. Some of the biomarkers analysts search for, include specific antibodies and endotoxins.
- Tissue biopsy. In this more intrusive examination, a “Ussing chamber” is used to evaluate a sample of your intestinal tissue. Ion transport through the intestinal barrier is measured using electrical current in the test. The ion transport measurement is parallel to water transport.
- Confocal endomicroscopy. This is an enhanced endoscopy exam that allows scientists to look at your intestinal lining in high resolution and magnification. A contrast fluid injected into your vein may show up in your gut if there is a gap in the lining.
How to heal leaky gut
What is the quickest way to heal your gut? The only known cure or treatment for leaky gut is to treat the underlying condition that causes it. Specific treatments for IBD, celiac disease and others associated with intestinal permeability have been shown to repair the intestinal lining in those who were affected.
On the other hand, treatments that target the intestinal lining independently have not been shown to improve these diseases or prevent intestinal permeability from recurring.
How to fix leaky gut
Heal leaky gut in 2 weeks: This entails increasing the consumption of vegetables, whole grains, and foods high in prebiotic fiber, as well as limiting the consumption of eggs, dairy products, and meat. Avoiding things like processed foods, added sugar, and artificial sweeteners. In order to increase the amount of good gut bacteria, add probiotics to your diet.
Leaky gut treatment
How can i take care of my gut health? Researchers are still looking into the advantages of different treatments for enhancing overall health and gut lining integrity. These therapies may not be able to mitigate a pathological disease, but they may help mitigate the effects of everyday factors such as diet, stress and bacterial overgrowth that can wear on your intestinal lining.
They may even help alleviate your general gastrointestinal symptoms. Therapies include:
- Probiotics. The capacity of certain probiotics to reestablish the function of the intestinal barrier is being examined individually. However, probiotics generally work to avoid an overabundance of the bad bacteria in your gut, particularly your small intestine, which may assist preserve the health of your gut lining.
- Prebiotics. Prebiotics provide nourishment for the good bacteria in your gut, giving them an advantage over bad bacteria. They are often plant fibers, which is another incentive to eat more vegetables.
- Eat less sugar and fat in your diet. These promote the development of the wrong types of gut bacteria and cause the production of abrasive dietary emulsifiers that may cause gut inflammation.
- Nutrition. Your gut may be strengthened by eating a balanced diet that contains all the essential macronutrients and micronutrients (vitamins and minerals). Your gut lining may in particular benefit from the use of vitamin D and the amino acid L-glutamine.
- Low FODMAP Diet. Because it methodically removes the majority of the typical food triggers, this particular diet is frequently recommended for persons with IBS and certain food allergies. By using it briefly, you may allow your gut the time to mend itself while learning which foods make you allergic to them.
Leaky gut supplements
Your microbiome is balanced and the harmful bacteria causing digestive problems are removed with the use of probiotics and prebiotics. Supplements for leaky gut may also contain additional active ingredients that may be therapeutic, such as curcumin, marshmallow root, vitamin D, licorice root, digestive enzymes, caprylic acid, zinc, and berberine.
Leaky gut diet
Eating foods, such as fruits, cultured dairy products, healthy fats, lean meats, fiber veggies, and fermented vegetables to help fight leaky gut.
What foods should I avoid with leaky gut syndrome? Avoid refined carbs, glutinous grains, white sugar, dairy products, vegetable oils, artificial sweeteners, alcohol, and caffeine if you have leaky gut syndrome.
Signs leaky gut is healing
How do you know if your gut is healed? Depending on your original symptoms, you can tell whether your leaky gut is healing if you notice that your bowel movements have stabilized, you no longer suffer from frequent episodes of constipation and/or diarrhea, your skin is healthy and radiant, and you have plenty of energy.
Bottom line
Numerous people experience hazy digestive problems, and the explanations are sometimes frustratingly unclear. In the lack of clear solutions, “leaky gut syndrome” has become a widely accepted diagnosis for dyspepsia in general and perhaps a wide range of additional disorders. True intestinal hyperpermeability, however, is too particular and intense to account for the symptoms of the majority of people.
The majority of patients only have nonspecific gut inflammation, which precedes intestinal permeability. This could be brought on by a specific disease or it might be the result of a variety of circumstances, including a poor diet, ongoing stress, and others. Consider making these changes. If it doesn’t work, consult a doctor. You can sift through the potential causes of your particular symptoms with the assistance of a trained gastroenterologist.
Also see: Intestinal Permeability: Symptoms, Test, Diet and Treatment
SOURCE: NEWFASTHEALTH CLINIC
Share: